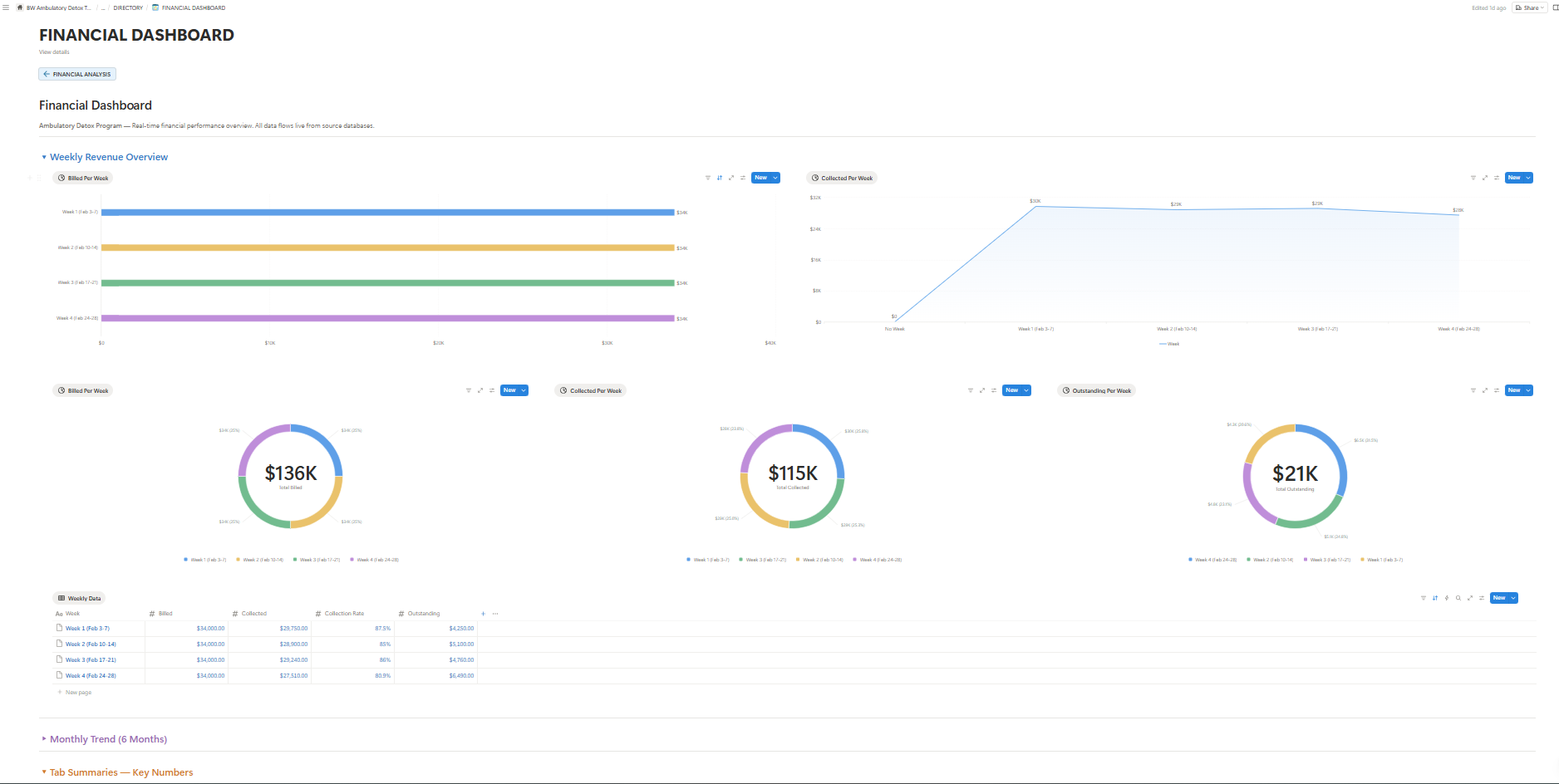
Walk into any behavioral health CFO's office in the country and you'll hear the same quiet frustration. Census is steady. Clinical outcomes are strong. The team is doing everything right. And yet, somehow, the year-over-year revenue line refuses to bend upward. The reason isn't a clinical problem — it's an operational one. And it's almost always hiding in the same place.
Across the engagements we run with outpatient programs, a single pattern repeats with near-perfect consistency: the detox phase of treatment — the highest-acuity, highest-reimbursement portion of the patient journey — is the most under-captured revenue stream in the entire facility. Not because the work isn't being done, but because the operational scaffolding around it was never built to capture it cleanly.
The number we see, again and again, is staggering. Up to 60% of clinically eligible detox revenue never reaches the income statement. Some leaks through documentation gaps. Some through admissions friction. Some through the silent attrition between intake and the first day of billable care. By the time the quarter closes, the gap is invisible — because it never showed up on the books in the first place.
The $690 Question
Every outpatient detox program in the United States operates within a roughly similar reimbursement band. Per-patient daily revenue varies by payer mix and state, but the working baseline most programs settle into is approximately $425 per patient per day — and the high-performing programs we work with stretch that figure considerably higher with proper documentation, clinical sequencing, and admissions discipline.
The delta between baseline reimbursement and properly captured detox revenue is not a marketing number. It's the operational headroom most programs walk past every shift.
Multiplied across a steady-state census, the difference between baseline and captured detox revenue compounds quickly. Three patients per week becomes meaningful margin. Five becomes growth capital. Ten becomes a different kind of business altogether.
Mapping the Revenue Curve
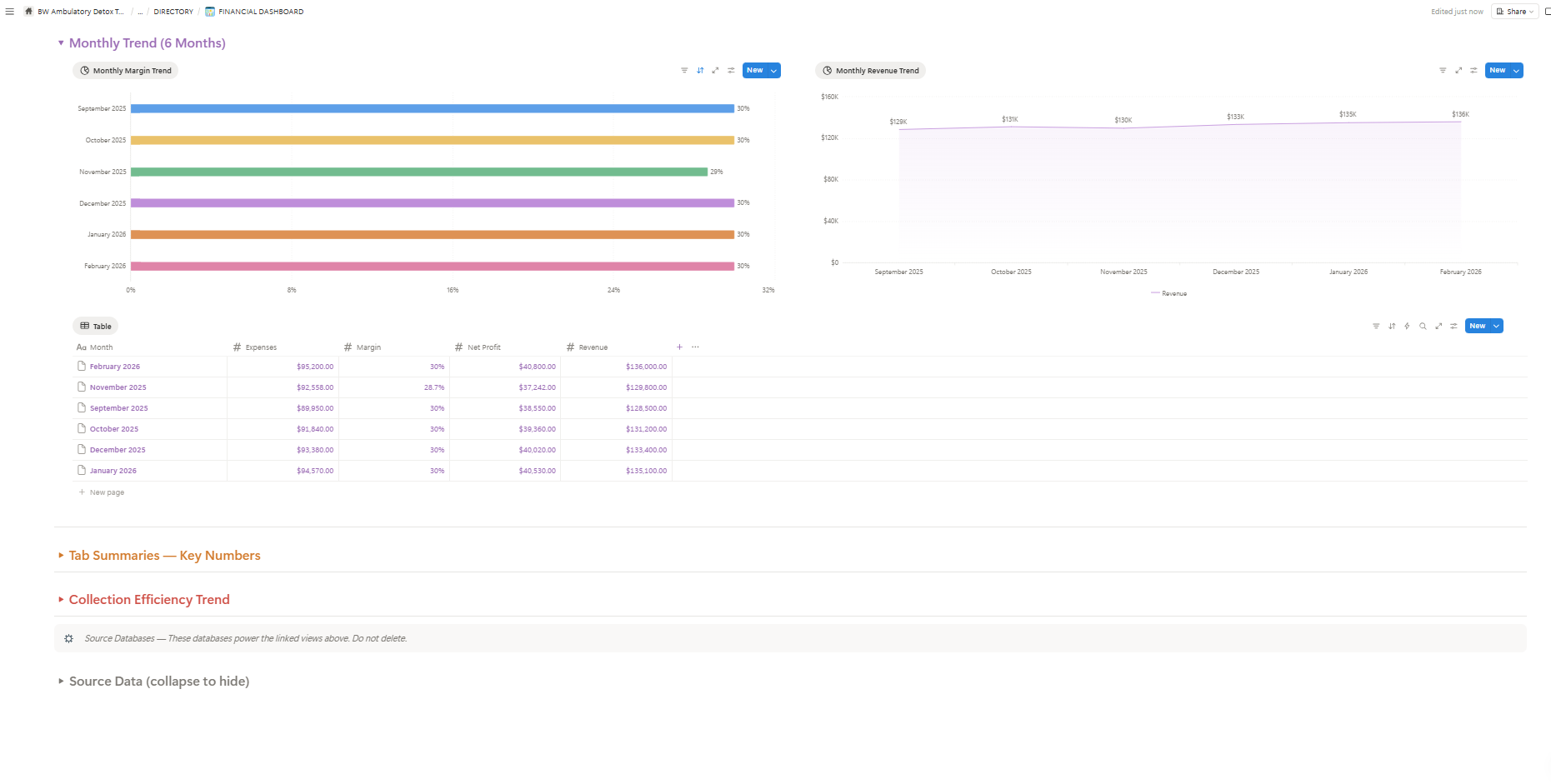
To make the math concrete, the table below models monthly revenue at three different weekly admission rates, holding length-of-stay and reimbursement constant. The numbers assume a clinically standard ambulatory detox episode and a properly captured per-diem rate.
| Weekly Admissions | Patients / Month | Revenue / Month | Annualized |
|---|---|---|---|
| 3 patients / week | ~13 | $38,000 | $456,000 |
| 5 patients / week | ~22 | $64,000 | $768,000 |
| 10 patients / week | ~43 | $127,000 | $1,524,000 |
Modeled at $425 baseline per-diem, standard ambulatory detox length-of-stay. Actual figures vary by payer mix, state, and documentation completeness.
The programs that capture this revenue aren't seeing more patients. They're seeing the same patients with better infrastructure underneath them.
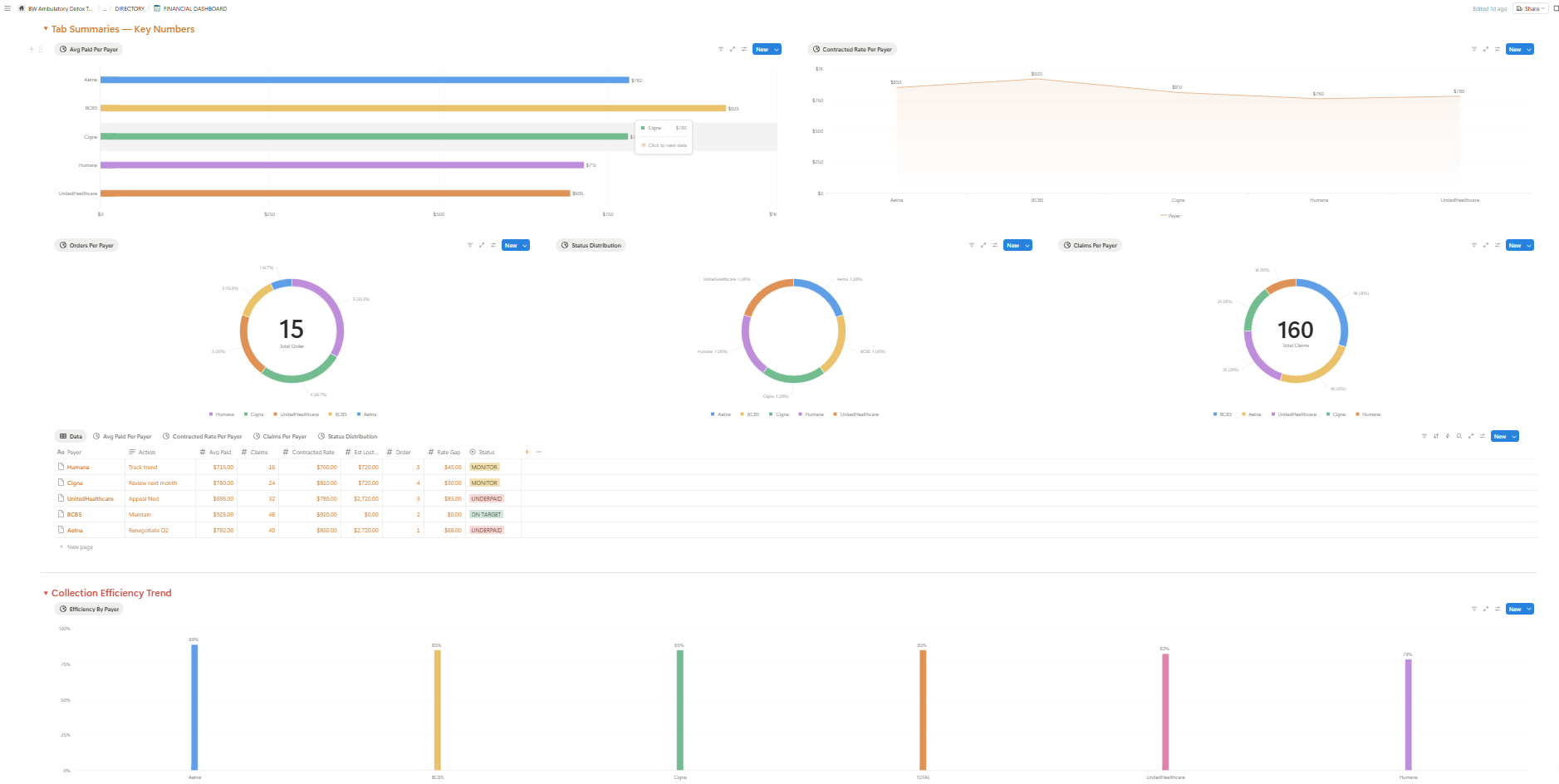
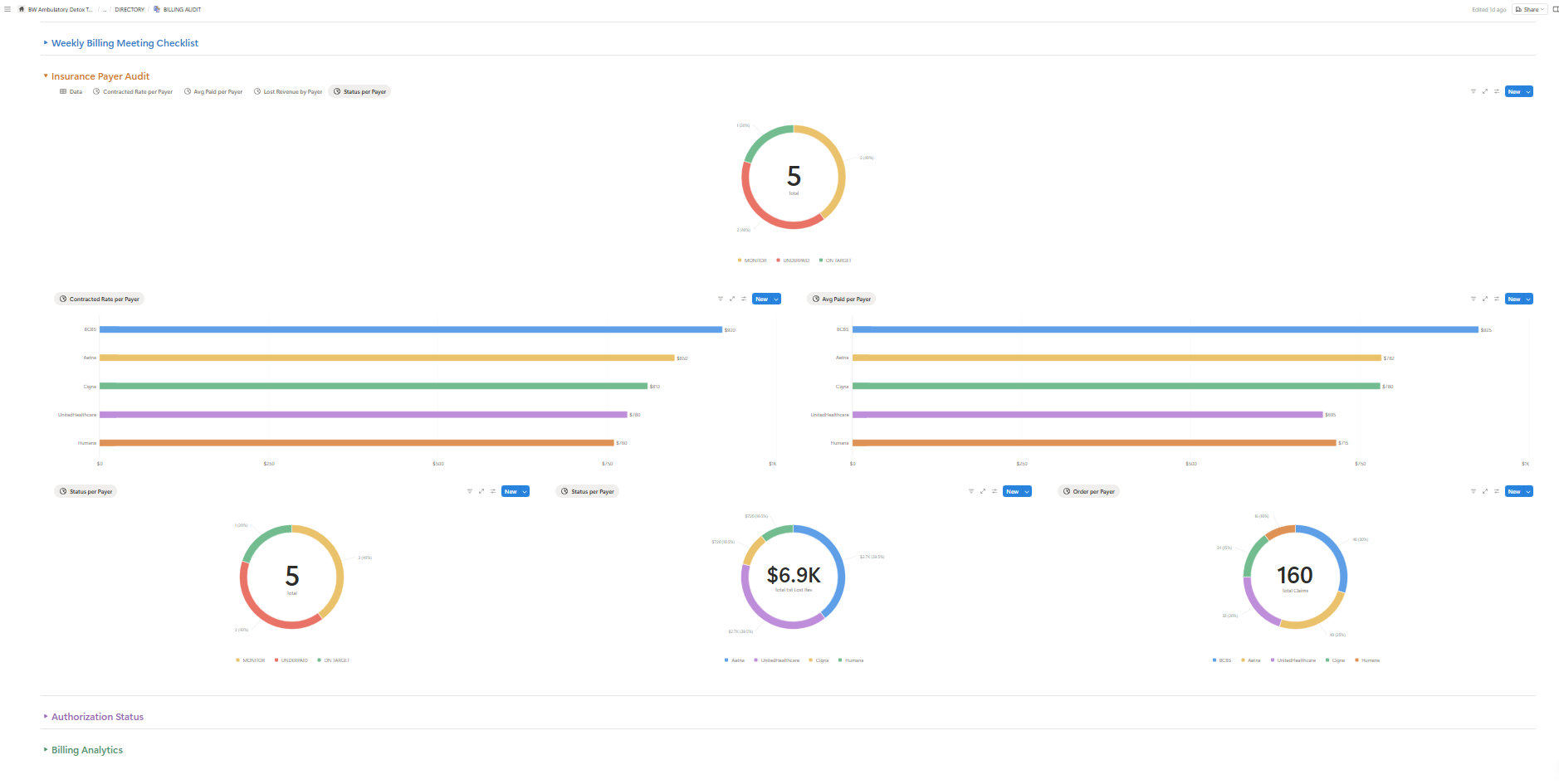
Where the Leakage Actually Happens
Across more than a hundred program audits, the points of failure cluster around four operational seams. None of them are clinical. All of them are recoverable.
- Admissions latency. The window between first contact and first billable encounter is where most clinically eligible patients quietly disappear. Friction in the intake workflow — verifications that take too long, paperwork that arrives at the wrong time, no after-hours response path — converts directly into unrecognized revenue.
- Documentation gaps. Detox-specific clinical justification is not the same as standard outpatient charting. The notes that satisfy a payer for IOP do not satisfy them for ambulatory detox. When the documentation framework hasn't been built around the acuity level, the per-diem doesn't get captured.
- CRM and EHR misalignment. Most programs run a CRM that doesn't talk to their EHR, which doesn't talk to their billing system. The resulting reconciliation gap quietly absorbs revenue that was earned but never recognized.
- Outcome tracking that informs nothing. Outcome data exists in most programs. It's almost never wired back into the admissions and clinical workflow in a way that improves either. That feedback loop is where compounding margin lives.
The revenue gap is rarely a sales problem. It's a sequencing problem. Programs that fix the sequencing — admissions, documentation, billing, outcome capture — typically recover the gap within one to two quarters, without changing their clinical model or their referral pipeline.
What "Recovery" Actually Looks Like
Closing the gap is mechanical, not magical. It involves three coordinated workstreams running in parallel: an admissions infrastructure that captures patients during the high-intent window; a documentation framework that maps clinical acuity to reimbursement clearly; and a feedback loop that turns outcome data into operational adjustments instead of quarterly reports nobody reads.
The programs that move quickly typically see the first 30% of recoverable revenue return within sixty days, before any deeper system changes have been made. The remaining margin requires the infrastructure work — the part that's harder to do but easier to sustain once it's running.
The Compounding Effect
What's worth noticing in the math is the second-order effect. Recovered revenue isn't just additional margin in the current quarter. It funds the operational upgrades — staffing, technology, clinical capacity — that make the next quarter's margin easier to capture. Programs that close the gap once tend to keep closing it, because the system is doing the work that the team used to do manually.
Programs that don't close it tend to keep not closing it, for the same reason in reverse. The leakage becomes invisible, then normal, then assumed.
Where to Start
The fastest diagnostic is the simplest one. Pull last quarter's admissions data, last quarter's billing data, and last quarter's clinical notes. Compare them. The gap between clinically eligible detox days and billed detox days is the number to start with. Everything else follows from there.
For most programs, that single comparison is enough to surface the operational seams. From there, the work is sequencing — which seam to close first, which one to leave for later, which one your existing infrastructure can already support if it's pointed at the right problem.