Stop Leaving Revenue on the Table With Preventable Billing Errors
Our comprehensive billing optimization program covers every step from initial patient intake to final reimbursement — ensuring the best ICD-10 and CPT codes, reducing denials, and maximizing cash flow.
Request a Billing Audit →$690
MISSED PER QUALIFYING PATIENT
Induction period billing codes that are frequently missed — recoverable revenue hiding in your current claims process.
End-to-End Insurance Billing Optimization
Navigating insurance billing is complex and time-consuming. We handle the hard parts so your team can focus on patient care.
Initial Call to Admission Training
Training your team to effectively communicate with insurance companies and clients — ensuring accurate verification of benefits, authorization, and pre-certifications.
Treatment Process Management
Guidelines and training to ensure each stage of treatment is thoroughly documented, maximizing reimbursement opportunities at every step.
Financial Tracking Systems
Real-time monitoring of all insurance billing activity, ensuring timely and accurate payment collection with AI-powered oversight.
Claims Follow-Up
Best practices for follow-up on unpaid or denied claims, ensuring that no revenue is left uncollected. AI flags underpayments automatically.
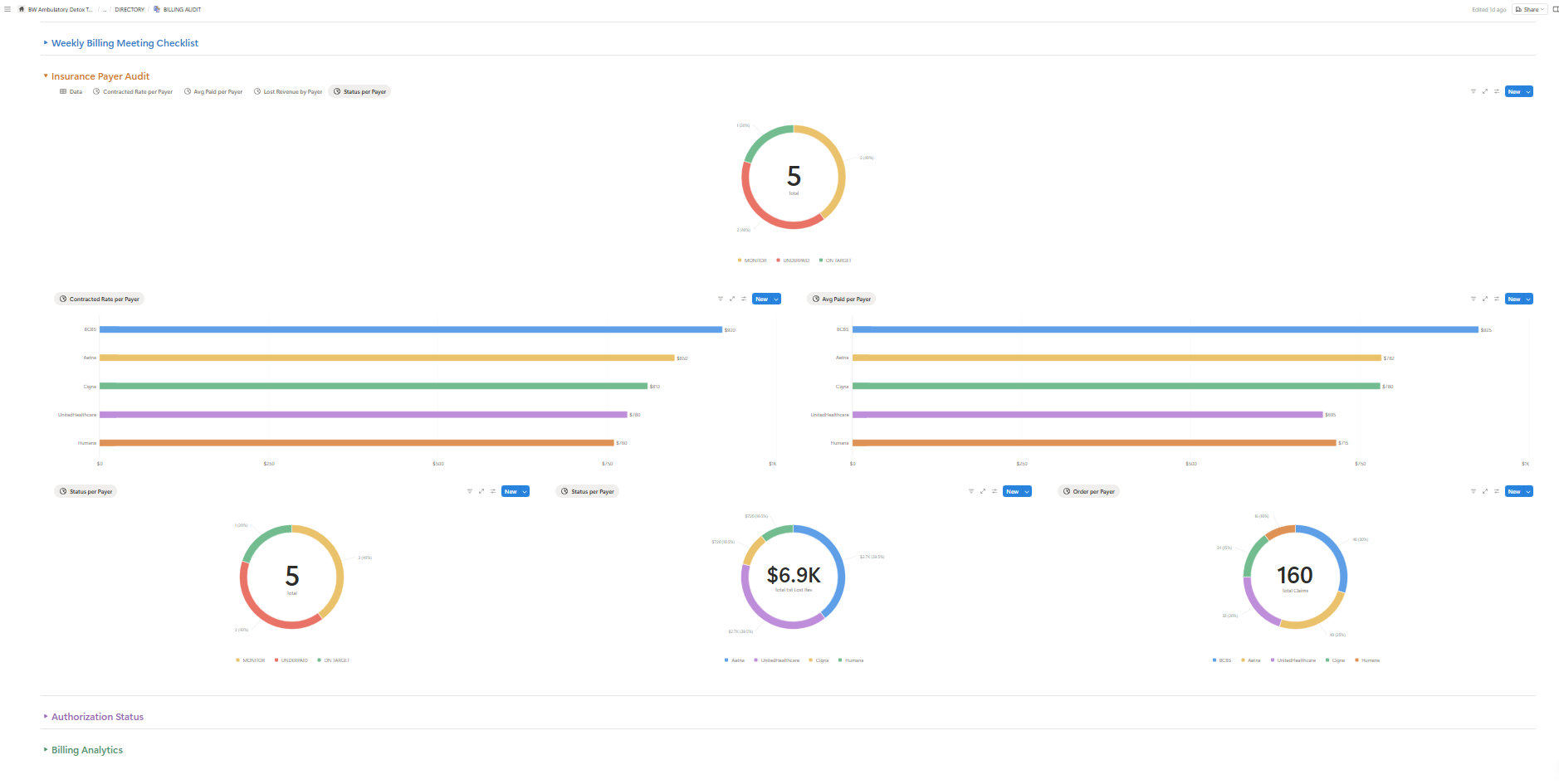
Every Underpayment Found. Every Dollar Recovered.
Our AI continuously monitors contracted rates against actual payments — flagging discrepancies the moment they occur, not months later during a manual review.
Contracted vs. Actual Rate Tracking
Every claim is compared against your contracted rates in real time. When a payer underpays, you know immediately — not 90 days later.
Automated Underpayment Detection
AI flags underpayments automatically and generates the documentation you need to dispute them — complete with contracted rate references and variance calculations.
Payer Performance Scoring
See which payers consistently underpay, delay, or deny. Use that data to renegotiate contracts from a position of strength.
Revenue Recovery Pipeline
Every flagged underpayment enters a tracked recovery pipeline with status updates, follow-up dates, and resolution documentation.
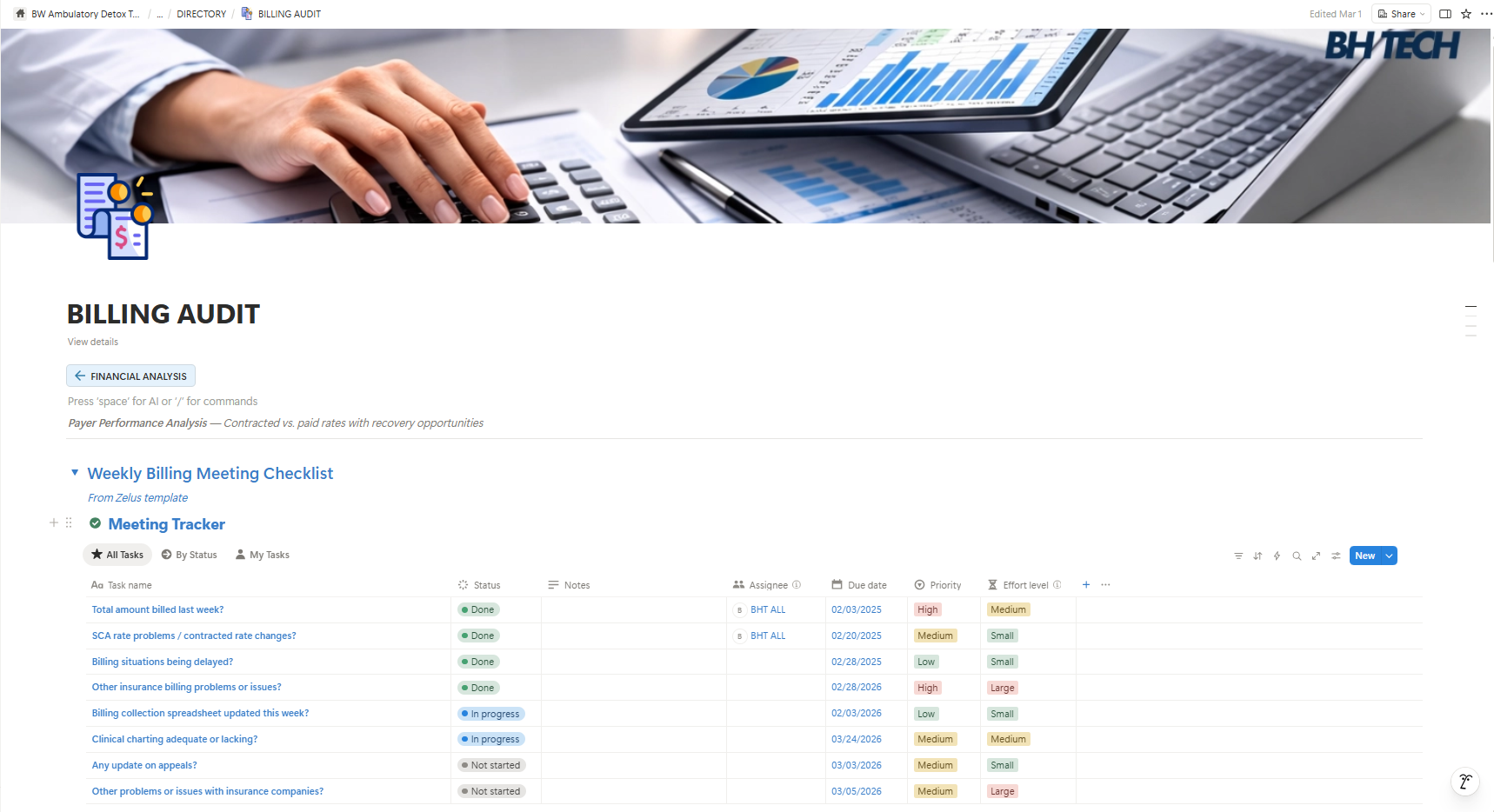
Reduce Denials. Accelerate Collections. Close Every Loop.
Most centers lose revenue not because claims are denied — but because denied claims are never properly followed up. We build systems that eliminate that gap.
First-Pass Approval
Correct ICD-10 and CPT code selection, proper documentation, and pre-authorization verification — ensuring claims are clean before they are submitted.
Denial Monitoring
Every denied claim is categorized by reason code, payer, and service type. Patterns surface fast — so you fix the root cause, not just the symptom.
Follow-Up Systems
Automated follow-up workflows for unpaid and denied claims with escalation timelines. No claim falls through the cracks, no revenue goes uncollected.
Streamlined Revenue Cycle, Stronger Financial Health
From intake to final payment, we optimize every step of your revenue cycle — and we have many opportunities for revenue cycle management across your entire operation.
Intake-to-Payment Optimization
Every step from patient intake through final reimbursement is mapped, measured, and optimized to reduce errors and increase accuracy.
Accelerated Cash Flow
Strategies to speed up billing and collections, reducing the time between service delivery and payment — so revenue hits your account faster.
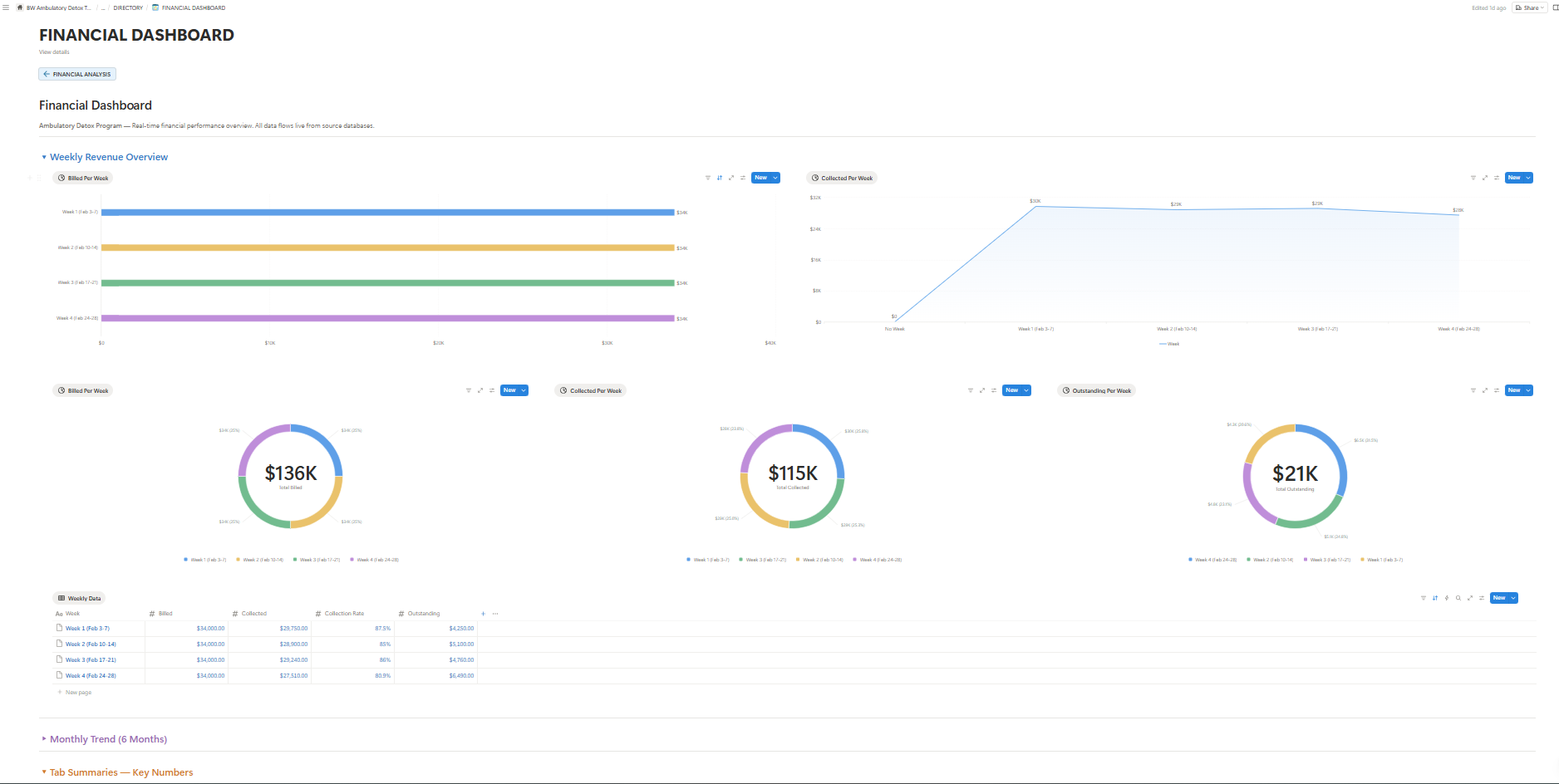
Real-Time Financial Dashboards
Live monitoring of all billing activity, claims status, collection rates, and payer performance. AI-powered oversight ensures nothing slips through.
Expert Behavioral Health Billers
Access to billing professionals with 30+ years of Medicaid experience and established relationships with major payer medical directors.
Billing optimization is our primary consulting service. We bring deep expertise in behavioral health billing, payer negotiation, and revenue recovery — backed by AI-powered tools and decades of industry relationships.
Know What Every Service Is Worth
Accurate billing starts with knowing the correct rates. These are the key billing data points your team should be capturing for every patient encounter.
The initial history and physical evaluation — a billable service that many centers undercode or miss entirely during the admission process.
The induction period carries specific billable codes that are frequently missed. Proper documentation and coding captures this revenue on every qualifying patient.
Each analyzer test is billable through insurance at approximately $79 per test. High-volume programs generate significant recurring revenue from this line item alone.
Rates are approximate and vary by payer, state, and contract. These figures represent typical reimbursement ranges our clients have documented.
Your Leadership Team Should Understand Every Dollar
Billing is not just for the billing department. Center leadership needs to understand revenue cycle performance, payer dynamics, and financial key performance indicators to make strategic decisions.
Dashboard Interpretation
Training leadership to read and act on financial dashboards — understanding what each metric means and when numbers indicate a problem.
Key Performance Indicator Management
Defining, tracking, and responding to the billing key performance indicators that matter most — collection rates, denial rates, days in accounts receivable, and payer mix.
Payer Negotiation Strategy
Using your outcomes data and billing analytics to negotiate better rates with payers. Know your value, document it, and present it effectively.
Revenue Cycle Oversight
Teaching executives to oversee the full revenue cycle — identifying bottlenecks, holding teams accountable, and making data-driven financial decisions.
Our network includes expert behavioral health billers with decades of Medicaid experience and established relationships with major payer medical directors.